Local association worried about staff shortages at Washington hospitals
Nov 13, 2020, 11:47 AM | Updated: 1:22 pm
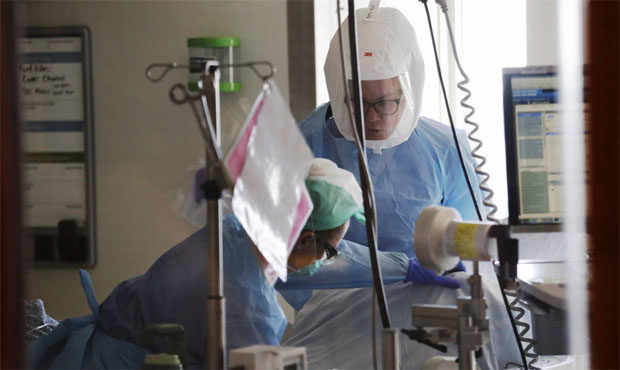
Health workers in Harborview's COVID-19 ICU. (AP Photo/Elaine Thompson)
(AP Photo/Elaine Thompson)
As hospitalizations rise in our state due to COVID-19, health officials are worried about hospitals reaching capacity.
King County Public Health Officer Dr. Jeff Duchin said on Tuesday that the health department is in close contact with health care workers to see how stretched the facilities are becoming. This, more than anything else, will determine if and when we get new COVID restrictions — and if hospitals start to get overwhelmed, these restrictions could be implemented suddenly.
“It takes weeks to turn around a trend, and if we see this trend is going in a direction that’s stressing our hospitals, we’re going to need to act pretty quickly,” Duchin said.
Beth Zborowski, senior vice president of Member Engagement and Communications with the Washington State Hospital Association, said the capacity of hospitals comes down to three factors — “stuff, space, and staff.”
“The supplies we need to take care of people, the space we need — the actual beds — and then the staff are the three things that we need to work in conjunction to be able to continue to keep the health care system up and running,” she said.
Of these, Zborowski said, staff is an especially large concern. That’s because the people working with coronavirus patients — ICU nurses and respiratory therapists — are highly-trained roles, and there simply aren’t enough of them to meet the demand caused by skyrocketing COVID-19 cases.
“ICU nurses and respiratory therapists are really specialized positions and we don’t have unlimited supply,” Zborowski explained. “We can’t just plug another person into those positions and have them be able to provide that level of care.”
During normal times, if one facility has a rush of critically ill patients, Zborowski said that hospitals can bring in staff through agencies from other states. However, that is not as doable right now, because hospitals across the country are all trying to stay afloat during the current surges in cases.
She added that health workers in the ICU have been going nonstop since the spring.
“They’re really tired and we want to make sure that we can keep them healthy,” she said.
While the pandemic months have seen layoffs and furloughs at major medical centers throughout the state due to the losses caused by elective surgeries temporarily stopping, Zborowski said those cuts are not why they’re worried about staffing. For one, most of the workers were temporarily furloughed and returned when elective surgeries started back up after the lockdown. Additionally, she said people caring for COVID patients were not let go because every one of those positions was needed.
“These specialized positions in the ICU were likely not as impacted, and they continued to be in demand, even during the shutdowns,” she said.
Over the next few months, Zborowski said, things are expected to get tight, as the “respiratory season” in hospitals that normally occurs every winter with increases in respiratory diseases combines with COVID-19. If medical facilities get too overwhelmed, non-urgent surgeries could be temporarily stopped again.
Ultimately, she said, we can each play a role in making sure hospitals do not get overwhelmed by “making sure we’re not their next COVID-19 patient.”
“We need to continue the social distancing, we need to continue to mask up and stop community spread, so that we can make sure our health care isn’t overwhelmed and we’re able to provide care to both COVID patients and regular emergencies,” she said.