Should the COVID vaccine go to the vulnerable first, or to super spreaders?
Nov 13, 2020, 1:35 PM
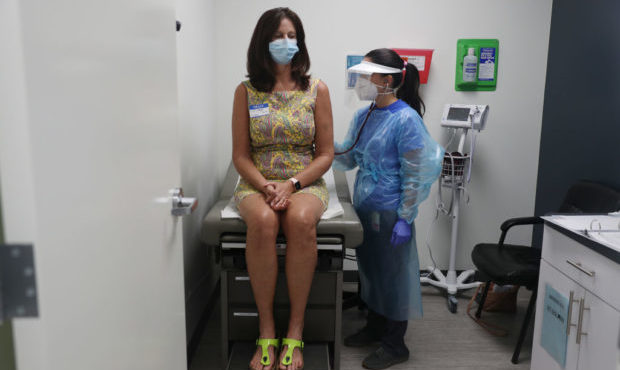
Barbara Corral, a Nurse Practitioner, conducts a physical on Lisa Taylor as she participates in a COVID-19 vaccination study at Research Centers of America on Aug. 07, 2020, in Hollywood, Florida. (Photo by Joe Raedle/Getty Images)
(Photo by Joe Raedle/Getty Images)
Health and Human Services have previously discussed that when a COVID-19 vaccine is available, it would go to the most vulnerable people first, including those in nursing homes, then frontline workers, and then to the general public. But what if there’s a more effective way to distribute the vaccine and stop the spread?
Local association worried about staff shortages at Washington hospitals
There’s an article on Wired that discusses the idea of giving the vaccine to super spreaders first, rather than giving it to older or more vulnerable populations.
“A bunch of people, top notch scientists with the CDC and WHO, World Health Organization, they haven’t come up with any final plan yet, but right now the tendency is not to do the obvious,” Tom Tangney explained, adding that the obvious is giving it to the most vulnerable. “They think maybe the most effective would be to go to the super spreaders. In other words, the people that are most … likely to spread it.”
Findings have shown, in all the outbreaks across the country and the world, it’s about 20% of people who are causing 80% of the cases, Tangney said.
“So the key is to stop the super spreaders. Stop super spreading events, of course, but also stop the super spreader, and that would be more effective,” he added.
It raises moral qualms, of course, and plenty of ethical questions, but the first challenge would be figuring out how to determine who qualifies as a “super spreader.”
The idea is that you talk to 10,000 people and determine the 150 names of people that keep coming up. Those 150 people are the super spreaders.
“Now, it’s certainly not airtight. It’s just a general hunch, and you may give it to people that don’t really need it because there are people that are very social and see a lot of people and don’t give it to people,” Tangney said. “So they’re not quite sure why that is, but still, in general, they’ll say that that would be a more effective way to stop the spread.”
The counter to this, Tangney continued, is that it’s a theoretical model that we don’t know if it would really work in real-life situations. The other side argues that it seems more certain to give it to the people who are facing death, in effect, rather than the people who have a better chance of catching and surviving this virus, as the majority of people do.
“Give it to the people that are absolutely most vulnerable because that’s a sure thing,” Tangney said, explaining the other side of the coin. “Rather than say, well, … this theoretical model says we don’t save the 85-year-old, we’ll give it to these hundred 58-year olds and hopefully that will stop the spread. So that’s the balance that’s being kicked around.”
John Curley suggests using phone data to help find the super-spreaders.
“The other way to track him down is you could use cell phone data be able to find super spreaders and the people that are congregating, moving around the most, and in other groups, they can track it and ping it and say, ‘OK, there’s a guy whose phone — that guy goes from here to here to here to here to here. He’s in this group, this group, this group,’ and then you’ll be able to track the data,” he said.
With Regal closing and delays, it’s as if 2020 didn’t exist for movies
The other problem though, as Curley points out, is that it’s been estimated that there are many more cases of COVID-19 than we know of now, which makes the spread all the more difficult to track.
“So if there’s 100 million people that have it, have had it, have it now, … gotten over it, that changes all the dynamics,” he said. “And then there’s far more people that are out there with this disease, then you wouldn’t be able to control it.”
“The problem is that [contact tracing is] no longer effective if it gets too big, too many of us have already have it, then contact tracing is irrelevant,” Tangney added, because then nearly everyone you talk to would have had it or would be in contact with someone who has been infected.
Read the full article from Wired that Tom & Curley reference online here.














