State warns COVID mental health struggles could get worse before better
Aug 1, 2020, 7:56 AM | Updated: Aug 3, 2020, 7:22 am

A closed park in Seattle in spring. (MyNorthwest photo)
(MyNorthwest photo)
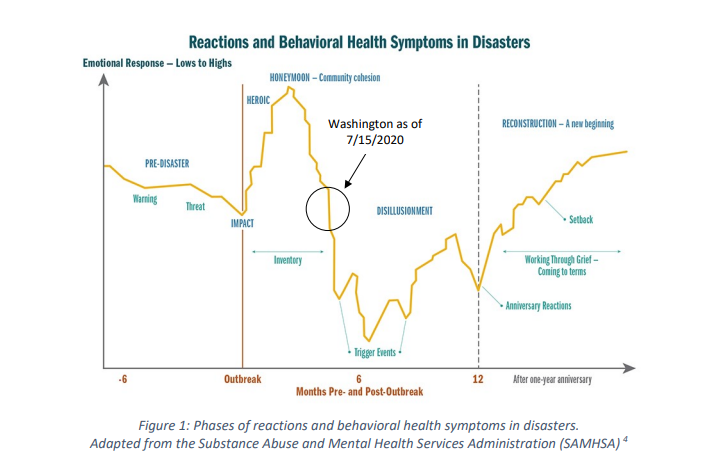
According to disaster psychology, we’re now entering the “disillusionment phase” of the COVID-19 disaster — and that means mental health struggles are likely only going to get worse for a while.
The Washington State Department of Health explained that during a disaster, people tend to start out in initial phases of optimism, with a desire to rally together, help each other, and celebrate teamwork and community spirit.
Now, however, we have passed the “heroism” and “honeymoon” stages, and, for the next few months, will be in the phase where anxiety and depression go up, as a feeling of helplessness takes hold.
In addition to anxiety over a deadly and uncertain virus, and depression over being stuck at home without seeing loved ones or taking part in favorite activities, Dr. Albert Tsai, a psychiatrist at Overlake Hospital in Bellevue, has seen some notable trends.
Struggling with mental health amidst coronavirus? Counselor offers tips
He said people who work at home may feel isolated — and those with kids, faced with being a worker, parent, and teacher all at once, can easily get overwhelmed. Contributing to the loneliness, Tsai said, is the fact that many places people go for comfort and support, such as community groups or religious centers, are closed right now.
It’s very important, Tsai said, to take mental breathers throughout the day with exercise, yoga, or meditation. Clearing your head, moving around, and getting fresh air for a little while can do wonders.
“Learning to take a break from school, or work, or your projects — making it essential that your mind takes a break,” he said. “Learning to not always have racing thoughts or be on the go, thinking that you always have to be productive or doing things.”
Cognitive behavioral therapy, which can be practiced through self-help books or with a therapist, can be very beneficial for those with anxiety.
Unfortunately, while exercise and nutritious foods go hand-in-hand with mental health, Tsai sees many people choosing to deal with anxiety and depression by self-medicating — in a variety of ways.
“When we talk about substance abuse, we might talk about chocolate, or fries, or eating more junk food — that is a substance as well. A lot of patients are reporting that they have less activity and more weight,” he said. “Alcohol consumption has gone up, typically, for a lot of people — it’s not an uncommon story that people say, ‘Yeah, I used to drink just one or two drinks, now it’s four or five in a week, or six to 12.'”
He said online alcohol sales are up 50-60% in stores, and 250% online; he also noted that gun sales are up. This combination together, he said, could lead to an increase in violent acts or even suicides.
First responders are also in danger of burning out with the immense pressure they face every day, Tsai observed. In some cases, health care workers have told him that being celebrated as a hero puts an even bigger burden on them every day, as they feel they cannot live up to expectations.
“I think it’s important that we come together as a community to not just praise people, but also find ways to have a disaster collectivism response, where we can really bond together as a community for things that will help us,” he said.
If a family member appears to be struggling with their mental health, Tsai said not to force them to talk about what’s bothering them if they don’t want. Simply show them you care by being there for them and providing a welcome distraction.
“I tell family members, ‘just be there’ — this culture that we have says we have to be doing something or talking about our trauma … but you don’t have to talk,” he said. “Sometimes just going for a walk, walking the dog, playing a board game, exercising together, eating together, even just sitting in the room together — just being there, spending time.”













